Managing Back Pain with Yoga
In your weekly yoga classes, you are very likely to find that most of your students will have experienced back pain at some stage in their lives. In fact, one in six Australians reports back pain, making it the leading cause of disability in this country and the most common reason for lost work productivity1. It is also the second most common reason people visit their GP2. With so many participants managing a back issue, even if they haven’t told you about it, yoga teachers are often well placed to help. Teachers can build comptence by understanding the current research, knowing the boundaries of scope of practice, and appreciating the remarkable therapeutic toolkit yoga provides. Ruth Gent from Dru Yoga offers the following educational prompts.
Red Flags and Referrals
Before anything else, yoga teachers need to be confident about when to refer a student to their GP. A red flag is a sign or symptom that may indicate a serious underlying condition. These are rare, and people experiencing them are unlikely to turn up to your class, but they matter.
Red flags include a history of cancer combined with unexplained weight loss or night pain, a recent trauma or risk factors for osteoporosis, fever with night sweats or signs of infection, and any symptoms of cauda equina syndrome such as urinary retention or saddle anaesthesia3. The Australian Journal of General Practice provides a detailed summary of these indicators for health professionals.
This highlights the importance of asking students to complete confidential health forms before they join your class and encouraging them to keep you updated about any health concerns. Although diagnosis or suggestions for medical management fall outside your scope of practice as a yoga teacher, there is a great deal you can address within a regular or specialised class and will be more confident to refer to the GP.
Active movement over passive strategies
The Australian Commission on Safety and Quality in Health Care released its Low Back Pain Clinical Care Standards in 20224, drawing on extensive research into how back pain is managed across the health system. The findings were striking. Despite strong evidence favouring active, low-cost approaches, many GPs still default to prescribing pain medication and ordering imaging. The Commission found that overuse of imaging and medication was associated with worse outcomes for patients, while education, staying active, and choosing non-drug therapies first led to better recovery5.
The Commission’s quick guide for GPs recommends supporting patients to self-manage their symptoms by prioritising active movement over passive strategies6. Yoga fits squarely into this picture as a modality that gives people time and space to learn about their bodies, build awareness, and gradually increase confidence in beneficial movement. The current medical consensus is clear on this point: backs need to move, and the sooner people with back pain return to gentle activity, the sooner they recover.
When is safe to start moving?
With acute low back pain in the first six weeks, gentle pain-free movement with a focus on breath is appropriate once inflammation settles. In the subacute stage from six to twelve weeks, loading can gradually increase as tolerated. For chronic pain beyond twelve weeks, regular and varied movement becomes therapeutic in itself, guided by pacing and symptoms.
Evidence from randomised controlled trials
Two randomised controlled trials at Bangor University investigated the effectiveness of a back care program based on Dru Yoga7. Compared to usual care, participants in the yoga program experienced statistically significant reductions in back pain.
In one six-month study of UK National Health Service employees, 56 staff who practised the Dru Yoga Back Care Programme for eight weeks reported only two sickness absence days due to musculoskeletal conditions, compared with 43 days missed by a control group of 53 staff over the same period8. These are compelling numbers for anyone considering a specialised back care offering, and well worth sharing with local GPs and allied health professionals who may refer patients your way.
Addressing Myofascia with Yoga
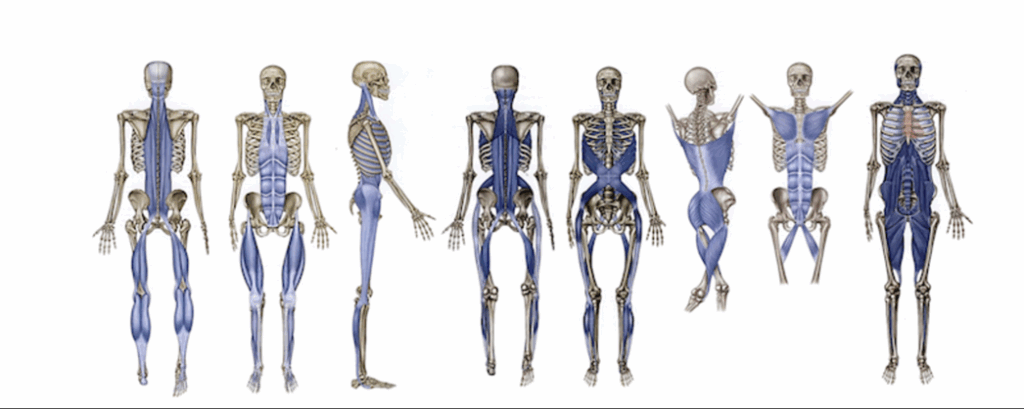
Fascia is the most abundant tissue in the body, spreading continuously from head to toe wrapping in and around all structures of the body from nerves, blood vessels, muscles and organs. Recent research has revealed that fascia plays a far greater role than previously understood. Containing over 250 million nerve endings it functions as a regulatory interface between the musculoskeletal, endocrine and nervous systems10. Together they create a dynamic, responsive whole body regulatory system creating harmony and balance.
Myofascia (the fascia around muscles, tendons ligaments and joint capsules) also contains a complex network of receptors for the autonomic nervous system, meaning it is intimately involved in stress response regulation and in emotional and mental wellbeing11.
When fascia is pliable and hydrated, we move smoothly, with ease and have a well- regulated nervous system. After injury, surgery, chronic stress and reduced mobility the fascia may become thickened, fibrotic, scarred and can contribute to pain, inflammation, stiffness and dysregulation of the nervous system.
Yoga postures and sequences performed slowly or dynamically, with long holds or rhythmic flow and awareness allows the myofascia to release, remodel and rehydrate resulting in greater mobility, reduced discomfort and a felt sense of spaciousness. In back care, addressing for example the thoracolumbar myofascia along the length of the back and into the sacrum can ease tension and decrease pain. Combining breath with movement through prāṇamaya kośa enhances the effect of these movements, helping to regulate the nervous system, improve fluid flow which may also help release emotions held within the fascia.
Addressing the iliopsoas muscle
The iliopsoas, part of the deep front myofascial line has been called “the hidden prankster” because it sits deep beneath the abdominal wall where most people cannot easily feel or connect to it. Although primarily a hip flexor, the iliopsoas links the upper and lower body alongside the quadratus lumborum, and dysfunction in this muscle can create tension through the sacro-lumbar area that results in lower back pain12. Given that the psoas major is contracted during times of perceived threat (either physical or psychological), it is a reservoir for holding trauma and stress through lingering tightness13.
Prolonged sitting allows the iliopsoas to habitually shorten, and a growing proportion of the population spends most of its day seated. In yoga classes, students with back pain benefit greatly from a good proportion of gentle floor work with postures that ease into the hips to stretch and release the iliopsoas and ease the surrounding fascia. Floor work also provides a sense of support and safety that enhances release of tension.
A helpful way to accommodate back care students in a regular class is to encourage students to choose between lying down for floor work or to remain standing or seated for the class, depending on their comfort. You can develop a wonderful student- centred approach where the choice to lie down or modify is normalised in class, enhanced by the kind permission-based language you use.
What is Trauma Aware Yoga?
Within the emerging world of using yoga to address emotional pain, trauma aware yoga introduces an awareness of how someone with trauma might need an attitude of care, invitation and respect for their personal space. It helps you notice signs someone with trauma might express and the thresholds that indicate you should refer them on for further help. Trauma sensitive and trauma informed yoga go further, exploring therapeutic ways to actively support someone in processing and recovering from trauma.
Addressing Belief Patterns with a Trauma-Aware Approach
We all tend to brace physically as part of the fear response to pain, injury and trauma. Back pain can be excruciating due to muscles that spasm in and around the lower back, even when there is no significant structural damage. Building confidence in movement again through a trauma-aware approach helps a person feel safe enough to relax, down-regulate their sympathetic nervous system, and allow muscles and fascia to reset into optimal function.
Professor Peter O’Sullivan, a physiotherapist at Curtin University, has conducted extensive research into belief patterns associated with chronic back pain14. His work identifies a range of unhelpful beliefs that increase fear-avoidant behaviours and can worsen pain over time. Common examples include the belief that back pain always indicates something serious, that getting older inevitably causes back pain, that scans will reveal the cause, and that pain during movement means harm is being done. O’Sullivan’s research shows how these beliefs lead to greater disability, work absenteeism and medication use.
As yoga teachers, we can help students gently reframe these patterns. Giving choice, encouraging a gentle approach and fostering self-determination about how much to do in each session all contribute to building the confidence that allows healing.
The language we use in class, the warmth of the environment we create, and the permission we give to students to work at their own pace are all part of this therapeutic process.
Bringing It All Together
Yoga teachers have a remarkable toolkit for addressing both the physical and psychological dimensions of students with back pain. Through targeted myofascial movements, breath work, nervous system regulation practices and a trauma-aware approach we can offer something that aligns with the best current evidence and fills a real gap in how back pain is managed across the health system.
If you are considering developing a specialised back care class, the research is firmly on your side. Let your local GPs and allied health professionals know what you can provide. You may find that a well-structured yoga back care program becomes one of the most rewarding aspects of your teaching practice.

DRU BACK CARE & MENTAL WELLBEING
Advanced training for yoga teachers to support back health, resilience and mental wellbeing.
50hr Accredited
Professional Development
Live Online
May – Aug 2026
About the Author
Ruth Gent is the Courses Director for Dru Australasia. Ruth teaches Dru Yoga & Meditation Teacher Training courses throughout Australia and New Zealand and mentors members of the Dru teaching teams. She is also a trainer on the Dru Yoga Therapy Course and is passionate about taking Yoga Therapy forward in Australia.
References
- Australian Journal of General Practice, RACGPs, Volume 53, Issue 9, September 2024. https://www1.racgp.org.au/ajgp/2024/september/best-practice-care-for-acute-low-back-pain ↩︎
- Australian Journal of General Practice, RACGPs, Volume 53, Issue 9, September 2024. https://www1.racgp.org.au/ajgp/2024/september/best-practice-care-for-acute-low-back-pain ↩︎
- Australian Journal of General Practice, RACGPs, Volume 49, Issue 11, November 2020. ↩︎
- Australian Commission on Safety and Quality in Health Care (ACSQHC). Low Back Pain Clinical Care Standard, 2022. www.safetyandquality.gov.au/publications-and-resources/resource-library/low-back-pain-clinical-care-standard-2022 ↩︎
- ACSQHC, Low Back Pain Clinical Care Standard, 2022. ↩︎
- ACSQHC, Quick Guide for GPs: Low Back Pain Clinical Care. https://www.safetyandquality.gov.au/sites/default/files/2022-09/low_back_pain_ccs_-_quick_guide_for_general_practitioners.pdf ↩︎
- Hartfiel, N., Burton, C., Rycroft-Malone, J., Clarke, G., Havenhand, J., Khalsa, S.B. and Edwards, R.T. (2012). “Yoga for reducing perceived stress and back pain at work.” Occupational Medicine, 62(8):606–612. ↩︎
- Hartfiel, N., Edwards, R.T., Phillips, C. (2014). “The cost-effectiveness of yoga for preventing and reducing back pain at work: trial protocol.” Journal of Yoga and Physical Therapy, 4:161. ↩︎
- Tom Myers Anatomy Trains. Photo: https://structuralbodywork.co.uk/wp-content/uploads/Anatomy-Trains-Myofascial-Meridians.png ↩︎
- Slater, D., Barclay, J. and Granfar, R. “Fascia as a regulatory system in health and disease.” PubMed Central, Frontiers in Neurology. ↩︎
- Patel, T.J. and Lieber, R.L. (1997). “Force transmission in skeletal muscle: from actomyosin to external tendons.” Exercise and Sport Sciences Reviews, 25:321–363. ↩︎
- https://evolutionsannapolis.com/iliopsoas-syndrome-hidden-prankster/ ↩︎
- Kelsey Loupy, phD Online Article Jul17 2024 Integrative Psychiatry. https://psychiatryinstitute.com/releasing-trauma-and-stress-with-the-psoas-muscle/ ↩︎
- O’Sullivan, P.B. “Back to basics: 10 facts every person should know about back pain.” British Journal of Sports Medicine, Volume 4, Issue 12. ↩︎



